Waterborne diseases surge among Vanuatu children after cyclones
Hospitals were already dealing with a rise in acute gastroenteritis when Judy and Kevin hit and cut supplies of clean water.

Port Vila, Vanuatu – A month after Cyclones Judy and Kevin spread devastation and flooding across the islands of Vanuatu in the southwest Pacific, water-borne diseases are escalating among children in the capital, Port Vila, and in rural communities.
Hospitals and health facilities are struggling to cope with the surge in cases as they continue to repair the damage caused to their facilities by the storms.
Keep reading
list of 4 itemsState of emergency declared as two cyclones hit Vanuatu in 24 hrs
Tropical Cyclone Judy hits Vanuatu, with another on its way
Tsunami warning withdrawn after powerful earthquake hits Vanuatu
“Prior to the cyclone, we were experiencing a surge of acute gastroenteritis. That was two weeks prior to the cyclone. After the cyclone, the numbers just shot up and increased. Initially, one-third of the children’s ward was full with acute gastroenteritis patients but that has increased to 50 percent of the ward bed capacity,” Dr Orelly Thyna, head of paediatrics in Vanuatu and chairwoman of Port Vila Central Hospital’s emergency operating centre, told Al Jazeera.
The ward, which has beds for 22 children aged 13 and under, is now accommodating up to 30 sick young children at any time. As more patients arrive every day, hospital management has been asked for extra space, Dr Thyna added.
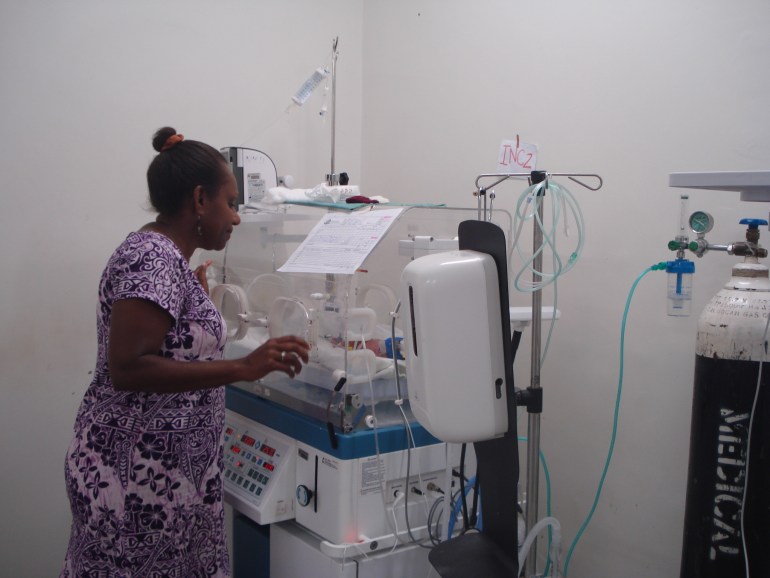
The children’s wards at the hospital suffered serious damage during the disasters. “We had flooding inside the children’s ward and it wasn’t safe for the children. In the neonatal intensive care unit, the roof was blown away, so we had to move the babies away to somewhere safe. That, in itself, is a challenge with all the traumatising effect on the parents and families,” Dr Thyna said.
Cyclones Judy and Kevin, which hit Vanuatu at the beginning of March, affected 80 percent of the Pacific island nation’s population of more than 320,000 people, including 125,500 children, according to Vanuatu’s National Disaster Management Office.
On Efate island, where the capital is located, widespread damage and destruction of homes forced many people into temporary shelters and evacuation centres. Communities were left without electricity and clean water after the storms, heightening their exposure to food and water-borne illnesses.
It was evident that “it was becoming more difficult for families to access fresh water as the electricity wasn’t working in many parts and is still not working in all parts of Efate Island. The pumping of water to homes was not reliable and drinkable water and water for household use is not universally available for everyone,” Jack French, Save the Children’s acting Country Director in Vanuatu, told Al Jazeera. The international children’s non-government organisation is helping with emergency response, aid distribution and recovery on the island.
In Erakor village, on Efate’s south coast, electricity and the piped water supply to the local health dispensary have been restored but staff are working to contain disease outbreaks under challenging conditions. The health clinic serves about 12,000 people living in surrounding communities.
Berry, the nurse-in-charge, told Al Jazeera that in children, “acute respiratory infections have increased along with skin infections and gastroenteritis. The cases of gastroenteritis are mainly due to people eating foods that have not been washed and hygiene practices which have dropped. Some children are suffering from multiple infections.”
He added they were also facing a shortage of some medicines. “We have run out of zinc tablets, which are used to treat gastroenteritis. The central medical store in the country has also run out of the tablets, so we are waiting for new supplies.”
Subsistence agriculture
Vanuatu has made significant progress in reducing the mortality rate for children under five, which is 23 deaths per 1,000 live births, compared with a global average of 38 per 1,000, according to the World Bank. However, diarrhoea remains a significant cause of death in young children worldwide, including in the Pacific Islands, reports UNICEF.
In one of the villages in the Erakor area, Rebecca told Al Jazeera that a scarcity of water, food and shelter was affecting her life and that of her family, which includes seven grandchildren – the youngest just two years old.
In the village, 200 people live in 150 homes, of which 55 need repair or rebuilding. Rebecca’s home consisted of two buildings but one has been destroyed. She is staying in a partially-constructed shelter with 10 other displaced locals
“We are sharing one rainwater tank with another family. The garden crops were destroyed. Some of the bananas survived but they are now finished, so we will have to find the money to buy food,” the 53-year-old told Al Jazeera. “And the children have skin infections and diarrhoea sickness.”
Vanuatu is heavily exposed to extreme weather and climate disasters. The World Health Organization has already warned of the health risks linked to climate change. Cases of diarrhoeal illness in particular tend to increase with drought and extreme rainfall.

The disasters are also affecting the resources people need to access health services. “Vanuatu is a subsistence agricultural society and the money earned from the agriculture that is sold is spent on transportation, getting children to school and paying to get to the health clinic. So with the destruction of a lot of home gardens and local farms, the inability [of families] to sell surplus agriculture is going to have an impact on health,” French said.
National recovery from the recent cyclones is expected to take several years. The health recovery of children in the country will require monitoring, say local experts.
French said that resuming school was key to supporting children’s resilience. Regular health monitoring of infants is also a priority, Sherold Sakita, Save the Children’s Early Childhood Co-ordinator, added.
“In terms of early childhood development, there is a challenge in that not all children are attending the maternal and child health clinic and we have identified children who haven’t had their immunisations,” Sakita said.
The Ministry of Health hopes to launch a school health screening programme, so that a broad range of potential developing health problems can be identified early, Dr Thyna said. “It’s a practical way to capture issues that might be overlooked by parents or, for reasons, they do not bring in their children [to health facilities].”