Double virus trouble: When COVID-19 meets the flu season
Public health measures for coronavirus can help keep influenza cases down this year, experts say, but there are concerns about the overlap of the two viruses.

Editor’s Note: This series is produced in partnership with the World Health Organization (WHO).
As the Northern Hemisphere heads into winter, countries face the double threat of the annual flu season overlapping with the continuing coronavirus pandemic.
Keep reading
list of 4 itemsWhere are we in finding a treatment for COVID-19?
Rapid coronavirus testing: A game-changer?
World pandemics
Influenza cases typically see a spike from November to March in the Northern Hemisphere and from June to August in the Southern Hemisphere – coinciding with cold weather conditions. In tropical and subtropical countries, there is no marked cold season, so flu tends to circulate all year round.
The WHO has warned that the co-circulation of influenza and COVID-19 – both of which cause respiratory illness – could place an additional burden on vulnerable populations and healthcare systems that are already stretched because of the pandemic.
To alleviate some of that strain, the UN health agency is urging countries to prioritise their influenza vaccination programmes this year, vaccinating those at high risk of developing complications – including pregnant women, the elderly, children, and people with underlying health issues. According to interim recommendations for the COVID-19 pandemic, if the flu vaccine is in short supply, two target groups – health workers and older people – should have the highest priority to get vaccinated.
There are currently no licensed treatments nor a vaccine for COVID-19, but several drugs and more than 200 vaccine candidates are being studied in large clinical trials.
“The good news is that there are ways to prevent and treat flu through vaccination, and antivirals for treatment, and also through the public health and social measures, which we’re using quite a lot for COVID that serve a purpose for both of them,” Ann Moen, chief of influenza preparedness and response at the WHO, told Al Jazeera.
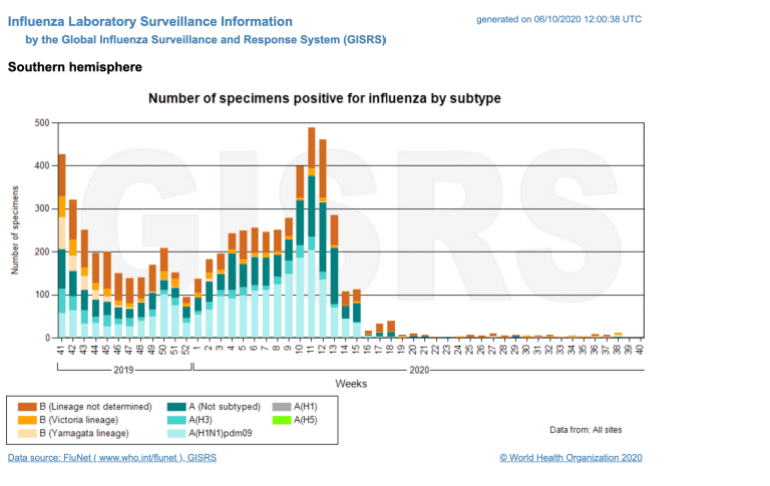
This year, countries in the Southern Hemisphere have already reported a significantly lower number of flu cases compared with previous years.
In Australia, for instance, a total of 21,156 lab-confirmed cases of influenza have so far been recorded by the department of health, compared with 289,731 flu cases over the same period last year.
Similar trends were seen during the peak winter months in New Zealand, South Africa and parts of Latin America.
Experts believe lockdowns, travel restrictions and school closures, as well as other infection prevention and control measures in place for COVID-19 – like physical distancing, hand-washing, respiratory etiquette and face masks – likely contributed to the downward trend.
But it remains unclear if a similar decline will be seen in the Northern Hemisphere in the coming months.
Moen said other reasons, like viral interference or viral competition, could be contributing factors and need to be studied further.
Similar symptoms
There are concerns about the overlap of the flu season with the COVID-19 pandemic, coupled with the similarities between the two viruses.
Both are transmitted by droplets spread through direct or close contact with an infected person, and indirect contact with contaminated surfaces, also known as fomite transmission.
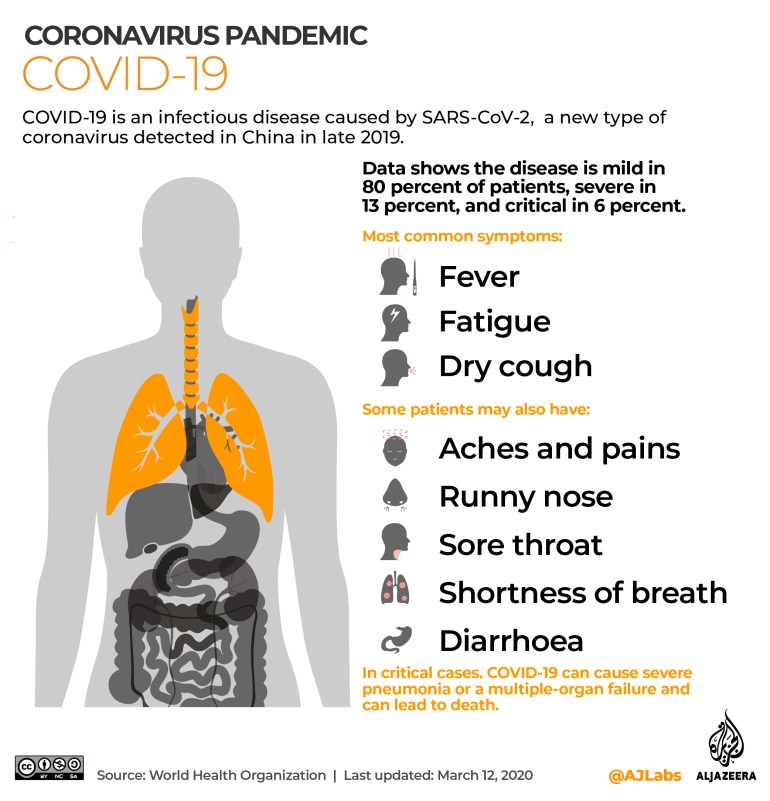
A person infected with COVID-19 or flu can experience their illness in a wide range of ways: from being asymptomatic or getting a mild case, to experiencing severe disease and even death. However, the greater mortality rate and higher fraction of severe and critical infections are seen in patients with COVID-19, according to current data and the WHO.
The flu and COVID-19 also have a similar range of symptoms – from fever, sore throat and dry cough to tiredness, headaches, and aches and pains.
However, a loss of smell and taste, especially among young adults, is more specific to COVID-19 patients.
“The only way to really know if somebody has the flu or COVID-19 is [through] a lab test. People can’t really self diagnose,” Moen said.
In all cases, people should follow local health guidelines, monitor their symptoms and seek medical care in case of severe illness, she added. And, if a person tests positive for COVID-19, it is important for them to self-isolate.
In a recent Q&A, Sylvie Briand, director of the Department of Global Infectious Hazard Preparedness at the WHO, said people with underlying conditions, such as cardiac disease or other respiratory chronic illness, asthma and diabetes, should be more aware of the signs of severity so they can get prompt advice and treatment.
Pregnant women are also at a higher risk of developing a severe form of influenza because of a change in their immunity. Where supplies permit, they should be prioritised to receive the flu vaccine.
The WHO will publish detailed guidelines to help countries better prepare and tackle the upcoming flu season amid COVID-19.
Follow Saba Aziz on Twitter: @saba_aziz